
CAREER PATHS
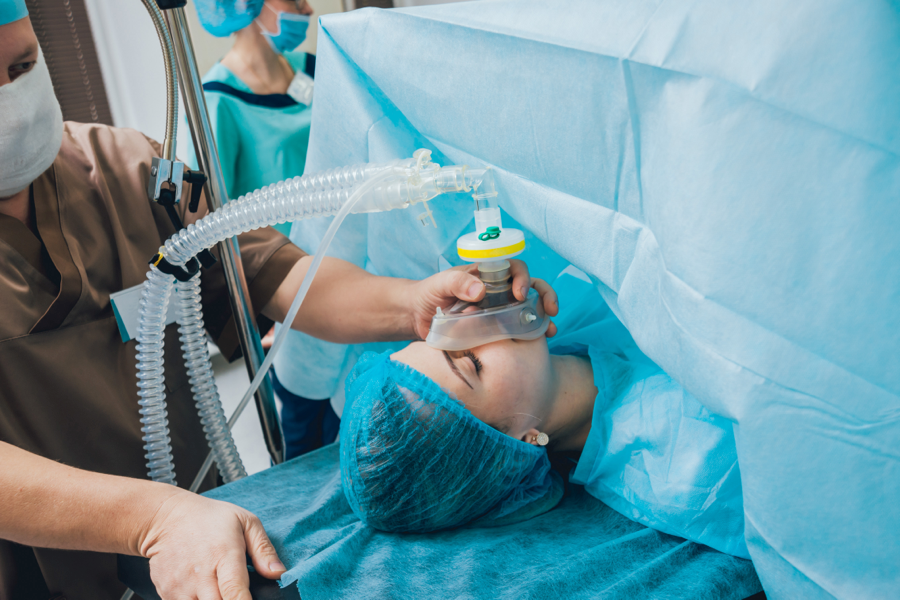
Nurse anesthetists and anesthesiologists are both healthcare professionals who adminster anesthesia. Both specialties provide intraoperative care for patients and enjoy a similar level of autonomy. To those outside the field it may seem like their overall responsibilities are basically the same. So, what are the differences between these two similar positions?
The reality is that these two career paths are very unique. CRNAs and physician anesthesiologists approach clinical practice from different models of care, and their education and certification requirements differ significantly. We will explore the differences between nurse anesthetists and anesthesiologists below.
There are significant differences between the education and clinical experience requirements of nurse anesthetists and anesthesiologists.
CRNAs are advanced practice registered nurses with a background in nursing. They typically hold a Bachelor of Science in Nursing (BSN) degree and have extensive clinical experience as registered nurses before pursuing a Master’s or Doctoral degree in Nurse Anesthesia (often a Master of Science in Nurse Anesthesia or a Doctor of Nurse Anesthesia Practice). CRNA programs usually take about 2-3 years to complete, and graduates are eligible to take the National Certification Examination to become certified CRNAs.
Anesthesiologists are medical doctors who have completed medical school (4 years), followed by a post-graduate residency program in anesthesiology (typically 4 years). Post-graduate training for an anesthesiologist typically includes a one-year postdoctoral internship, a three-year postdoctoral residency in anesthesiology, and may include an additional 1-2 years of education in an anesthesia subspecialty area.
It is estimated that physician anesthesiologists complete nearly double the education and 10 times the clinical training hours of CRNAs. After high school, it takes a total of eight to ten years and an average of 2,604 clinical training hours in a nurse anesthesia program to become a nurse anesthetist. After high school, it takes a physician anesthesiologist 12 to 14 years and 12,000 to 16,000 hours of clinical training, to enter practice.
CRNAs focus on the administration of anesthesia and the management of a patient’s pain during surgical, obstetrical, and various medical procedures. They work in collaboration with surgeons, dentists, podiatrists, and other healthcare professionals. CRNAs often work in hospitals, surgical centers, and outpatient clinics.
Anesthesiologists are physicians who specialize in perioperative patient care, which includes not only anesthesia administration but also pre-operative and post-operative patient assessment and management. They can also manage critical care patients in intensive care units. Anesthesiologists typically work in hospitals, but they can also work in outpatient settings, especially in pain management clinics.
CRNAs often have a high degree of autonomy in their practice, and in many states, they can work independently without direct supervision by an anesthesiologist. They can assess patients, develop anesthesia care plans, administer anesthesia, and monitor patients throughout procedures.
Anesthesiologists retain overall responsibility for the patient and is available to the CRNA throughout the case, but may delegate patient care duties to the CRNA or other qualified anesthesia personnel. For example, the CRNA may handle much of the pre-operative preparation and remain at the patient’s bedside throughout the procedure, while the physician is nearby.
The anesthesiologist works with the CRNA to develop the anesthesia care plan and monitors patients at critical junctures of their care, including the patient’s pre-op interview, during intubation, and emergence from anesthesia.
While CRNAs have a focus on anesthesia, they may also choose to specialize in areas like pediatric anesthesia, obstetric anesthesia, cardiac anesthesia, or pain management.
Anesthesiologists can pursue additional subspecialty training in areas like pediatric anesthesia, cardiac anesthesia, neuroanesthesia, pain medicine, and critical care.