
CAREER PATHS
A requirement for students in nursing school is participating in clinical rotations. In these rotations, nurses do not have the opportunity to experience specialty areas such as the Intensive Care Unit (ICU) or Emergency Room (ER). These specialties involve managing traumatic patient situations in a fast-paced setting.
Nurses often leave school wondering about the differences between an ICU and ER registered nurse. This article will explore all of the key differences.
Nurses in both of these settings are also lifelong learners. They follow industry trends and continuously educate themselves through certifications, seminars, and additional Continuing Education Hours. Regardless of the environment, nurses strive to become the best they can be.
Both nurses are required to collaborate in a team environment. Never truly working alone, nurses are expected to help out their coworkers when necessary. Otherwise, critical patients may suffer and nurses are more likely to become burnt out.
Remember “ER”? This classic show depicted a constantly chaotic and “always on” work environment. In reality, some days are quiet while others are extremely hectic. You never truly know what kind of day you will have—even at the start of your shift. The unexpected adrenaline rush is one of the reasons that many nurses love working in the ER.
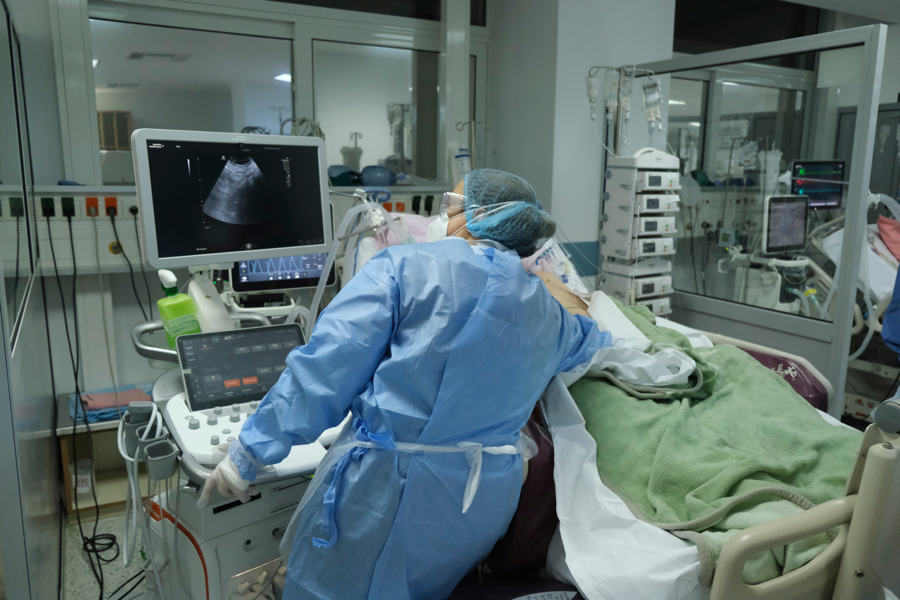
The ICU offers a more organized and calm environment. At times, patients are medicated and sedated due to their medical condition. Upon becoming stable (often called a “walkie-talkie” patient by nurses), they are transferred to a lower level of care.
ER nurses particularly love fast-paced situations. They start their day by triaging patients and assessing them to determine their priority of care. However, this can always be derailed if an ambulance arrives with a critical patient.
Depending on the patient’s condition during an assessment, the nurse may have to initiate a protocol. For example, a patient might be experiencing chest pain. Hospitals have chest pain protocols in place for the patient to be treated in a timely, evidence-based, and algorithmic manner.
The nurse notifies the physician, who then evaluates the patient and places orders. Next, the nurse implements the orders to provide treatment and stabilize the patient. She will then move them to another area of the hospital or discharge them.
As patients often need multiple medications and treatments, ICU nurses essentially act as a well-oiled machine with a time schedule. ICU nurses also assess and monitor patients, carefully following all necessary protocols. They wait for the ICU physician to round and place new orders. If the nurse notices a change in their patient, she will notify the physician and orders are then arranged over the phone. ICU nurses are responsible for administering the ordered medications and treatments.
An ER nurse’s primary goal is to stabilize the patient and discharge home or admit them to another area of the hospital.
In the ICU, the goal is for the patient to oblige with nursing orders, follow a designated carepath developed by the physician, and be transferred to a step down unit.
Unfortunately, death is an inevitable part of both settings. This occurs when patient stabilization is unsuccessful. Both ICU and ER nurses will need some time to grieve their patient’s loss—no matter how long they were in their care.
According to Indeed.com, ER nurses typically receive $45.01 per hour.
ICU nurses earn an average of $46.41 per hour.
This amounts to approximately $80,000 to $90,000 a year.
The differences in pay can vary from state to state. Due to the current global pandemic, many nurses are offered bonuses for frontline work in critical areas such as the ER and ICU.
It’s important for ER nurses to demonstrate flexibility, as they are required to take on patients quickly and turn them over to their home or another unit. If their assignment isn’t too heavy, they are expected to support their co-workers with more critical patients.
Some of the many types of typical situations in the ER include:
These patients require over 24 hours of critical care and need to be monitored by a nurse frequently.
Needless to say, registered nurses in the ER and ICU are highly knowledgeable and always up for a challenge. If you are still unsure about which setting is right for you, shadow a nurse in both areas and see which resonates best.